


Eradicating the skin cancer crisis for people with albinism
The Issue
From 2017 to 2019, rates of harmful skin conditions fell by 23% across our patient population
With over eight hours of intense sunlight a day, East Africa is one of the hottest places on Earth. Without the protective pigment melanin, people with albinism are highly vulnerable to skin cancer. Inadequate skin screening provision, lethally slow rates of diagnosis and an appalling lack of sun protection education, sunscreen, wide-brimmed hats and protective clothing have given epidemic prevalence to this otherwise preventable disease. One estimate suggests fewer than 10% of people with albinism in Tanzania survive skin cancer to reach the age of 30.
Standing Voice’s Skin Cancer Prevention Programme is an expanding network of regular skincare clinics reaching thousands of people with albinism in their own communities across Tanzania and Malawi. Over 8,500 people with albinism are reached by our programme, which operates at 150 clinic sites across Tanzania and Malawi. Prior to our services, the majority of those with albinism lacked access to adequate skincare, while the fortunate few receiving treatment faced an average waiting time of 14-17 months. Our patients now wait a maximum of 6 months. The Skin Cancer Prevention Programme is a blueprint to be replicated and expanded across Sub-Saharan Africa.
IMPACT
96% of our patients in Tanzania are returning regularly to clinics
9,518 patients reached by Skin Cancer Prevention Programme
Our clinical network operates at 199 locations
The Programme
SKIN CANCER AND ALBINISM
The sun emits ultraviolet rays. These rays cause skin cancer by interacting with genetic information (DNA) in skin cells and inducing oxidative damage. Melanin is a photoprotective pigment that interrupts the ability of sunlight to damage skin cells, absorbing UV rays and dissipating their energy as harmless heat. Albinism impedes the production of melanin, removing this natural defence against the harmful rays of the sun. As a result, people with albinism are uniquely susceptible to sunburn, and at elevated risk of developing skin cancers related to chronic sun exposure. They are particularly vulnerable to basal cell carcinoma and squamous cell carcinoma (though no more prone to melanoma than anyone else). Basal cell carcinoma develops in the bottom of the epidermis over a number of years, and is unlikely to invade surrounding tissue. Squamous cell carcinoma originates in the top of the epidermis, grows rapidly, and is more likely to spread to other areas of the body.
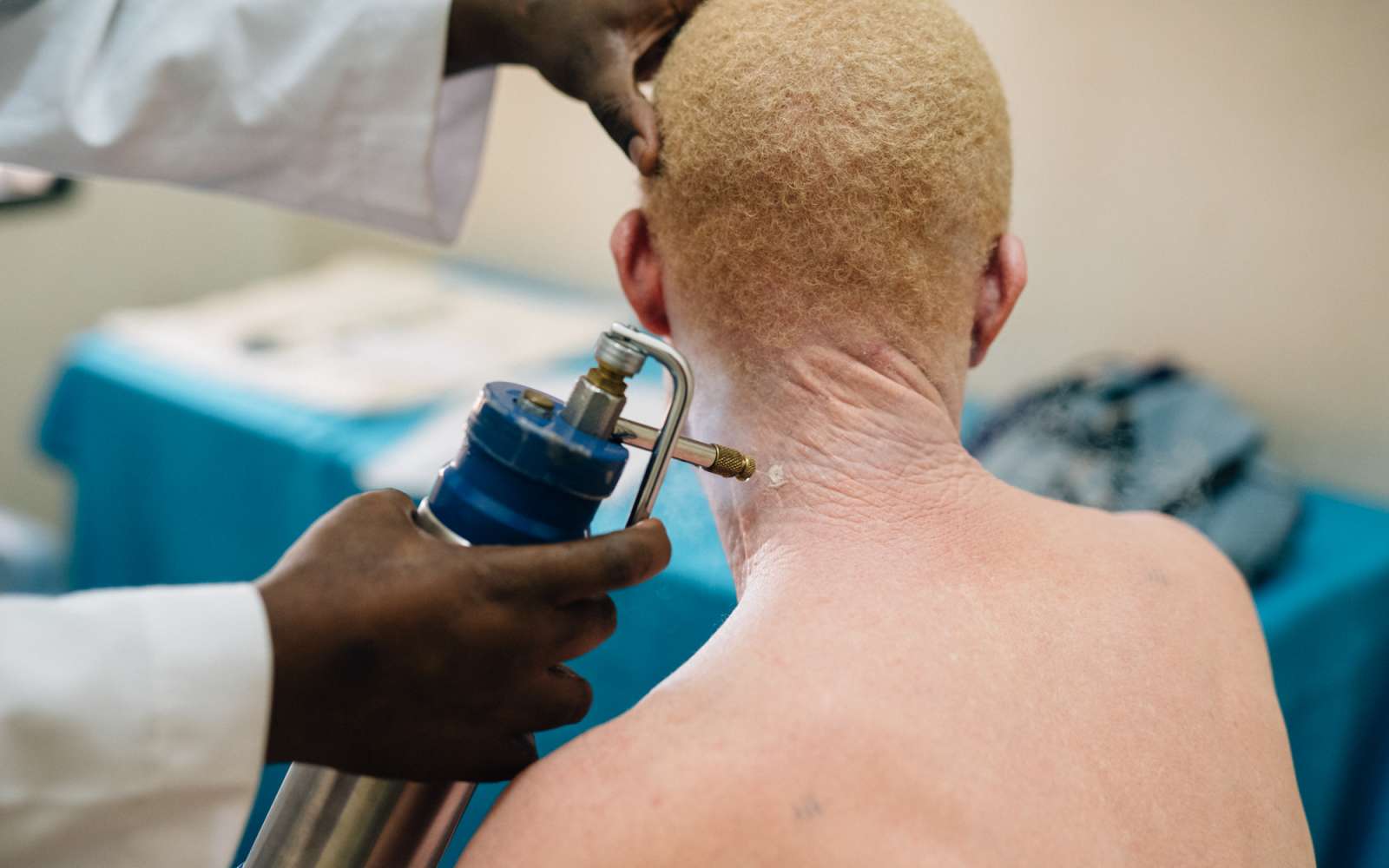
Lifetime exposure to UV radiation is the single greatest risk factor for developing skin cancer. Periods of high exposure or instances of extreme sunburn, especially in childhood, can precipitate the emergence of skin cancer later in life. If the disease does develop, early detection and intervention are critical: in many cases people with albinism develop pre-cancerous patches (actinic keratoses) that can be removed with liquid nitrogen cryotherapy before cancer occurs. Skin cancer is not always preventable, but the likelihood of acquisition can be reduced by minimising exposure to sunlight (particularly around midday), applying sunscreen, and wearing long-sleeved clothing and wide-brimmed hats outdoors. Because they lack the natural protection afforded by melanin, people with albinism must exercise particular vigilance in these areas.
In East Africa UV radiation is especially intense, further elevating the risk of skin cancer for people with albinism. In Tanzania social marginalisation and stigma combine to exacerbate this threat. In the past, dermatological care for Tanzanians with albinism has been insufficient. Until now, services have been sporadic, with limited geographical reach and no structured referral process, leaving many with albinism with poor screening provision and lethal delays in cancer diagnosis. Historically Tanzanian hospitals have struggled to address the needs of people with albinism. Hospitals have often lacked resources, rarely possessing the infrastructure or facilities to develop dermatology services. People with albinism seldom have the financial means to pay fees for skin cancer treatment: the vast majority of our patients have never seen a doctor about their skin when they first attend our clinics. This vulnerable population has been disconnected from doctors, hospitals and healthcare networks of any description. This has directly precipitated the epidemic we see now. Frequently marginalised from education and formal employment, people with albinism in Tanzania are also more likely to work as subsistence farmers, spending long hours outside in the blistering heat. Sun protection education is alarmingly rare in Tanzania, so people with albinism, and parents of children with albinism, are frequently ignorant of necessary preventative measures. Together these elements have produced an epidemic among this population, with one estimate indicating that only 10% of people with albinism in Tanzania survive skin cancer to reach the age of 30.
THE MODEL
Standing Voice combats this situation by activating, equipping and connecting existing networks of dermatologists and other stakeholders inside Tanzania to provide a regular clinic service to people with albinism across the country.
Our team has carefully structured the programme to provide: clear roles for every stakeholder; specific, realistic budgets; a well-defined strategy for data collection; comprehensive training for health professionals and a clinic service thoroughly equipped, monitored, and evaluated.
Costs are managed in line with government expenditure so that our programme can be easily absorbed into the country’s national health budget. While we do mobilise the skills of international experts to facilitate training, service delivery is always locally led.
For people with albinism, the entire service is free, reliable and consistent. Clinics are conducted locally in patients’ home communities every six months. With two dermatologists at each of our clinics, patients receive skin cancer screening and liquid nitrogen cryotherapy to remove any pre-cancerous wounds on site. Patients also receive Kilimanjaro Sunscreen (Kilisun), a thicker, stronger, Tanzanian-made sunscreen specifically designed for people with albinism; Standing Voice funds the production of Kilisun through the Kilimanjaro Sunscreen Production Unit in Moshi, Tanzania. Our clinics also educate people with albinism, as well as their families, teachers, and wider community members, to manage their health needs. Dermatologists provide practical education on how to limit UV exposure with protective clothing, wide-brimmed hats and Kilisun, and explain how to monitor dermatological health through self-examination. In locations where clinics have been running longest, reductions in the presentation of skin cancer have been as high as 85%.
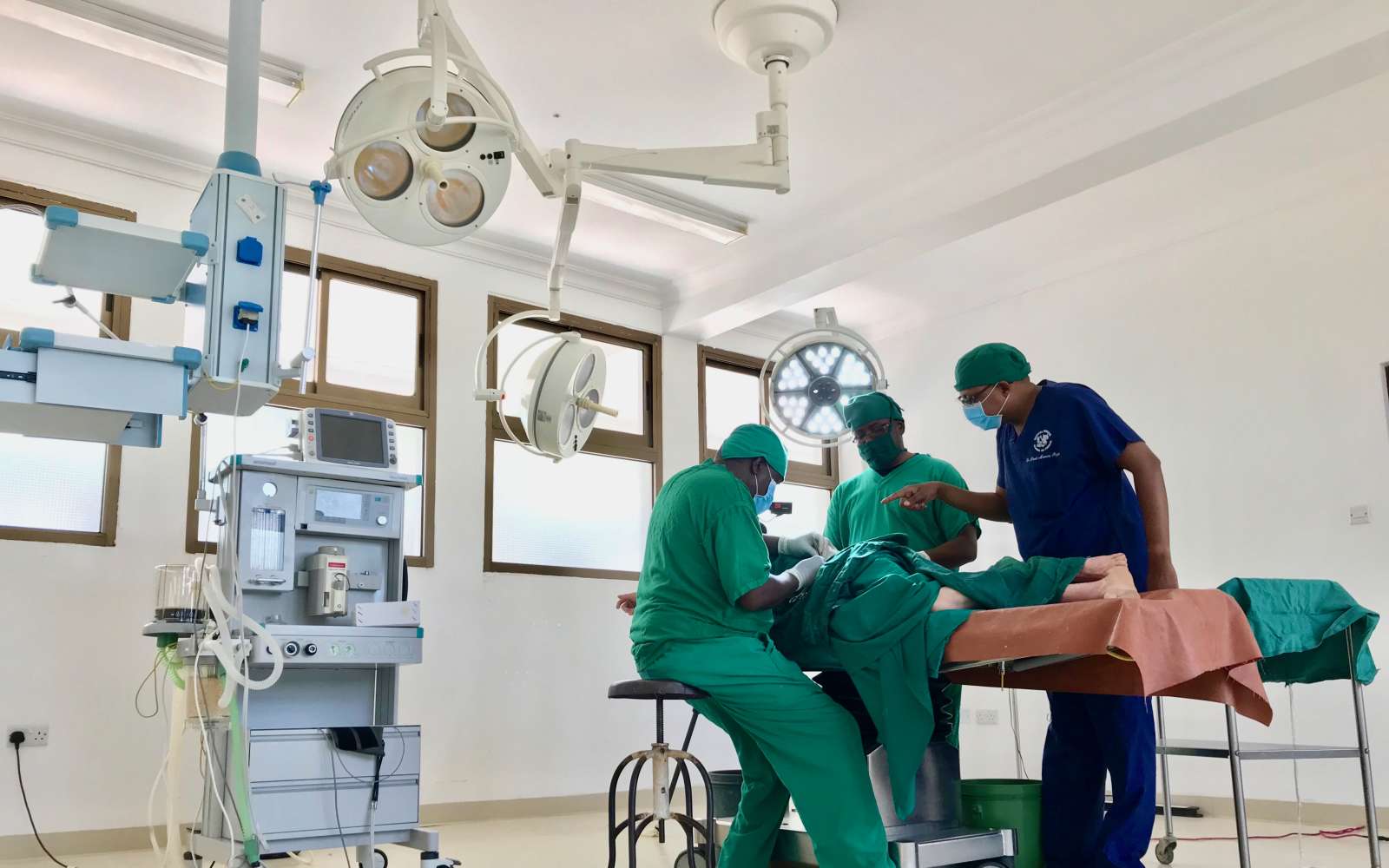
Following critical data collection, any patients presenting advanced cancerous wounds are referred to the relevant hospital for emergency surgery, an urgent medical service unavailable before our programme. Our team coordinates and funds the patient referral process, covering travel to (and from) the relevant referral hospital and the cost of treatment itself. After surgery, we arrange for patients to stay in safe, comfortable environments before ultimately returning home. Between clinic cycles we follow up with patients to identify any changes in dermatological health, making surgery referrals where necessary. Crucially, we fund surgery training for Tanzanian dermatologists to expand our network of in-country referral hospitals.
Our clinics are already witnessing significant strides toward replication and handover, with some district governments now covering selected costs in their areas; providing transport for patients to attend; securing hospital space; and offering their own health professionals as supporting staff. The Ministry of Health has formally endorsed the Programme, while the UN Independent Expert has recognised the programme model as a form of best practice, and delegates from 29 African states have issued formal requests for the replication of the Skin Cancer Prevention Programme in their respective countries. The Programme has quickly established itself as a leading model of dermatological healthcare for people with albinism in Tanzania. Building on this success, the Programme has now been fully replicated in the Mangochi and Machinga districts of Malawi, with 457 patients now registered.
Our programme offers people with albinism a structured, regular service, run in multiple areas by our local teams and partners. It follows Standing Voice’s blueprint of engaging in-country individuals and groups to produce sustainable, lasting change: we work with governments, healthcare professionals and civil society organisations so that so that individuals and institutions in Tanzania and Malawi are equipped to manage the skin cancer crisis. The bare ingredients of adequate healthcare for people with albinism in Tanzania and Malawi already exist: our programme brings these ingredients together.
Programme partners include: the Regional Dermatology Training Centre; community dermatologists; the Skin Cancer Advisory Committee; the Tanzania Albinism Society; the Association of Persons with Albinism in Malawi; schools and centres; hospitals; the Ministry of Health and the government; the Kilimanjaro Sunscreen Production Unit; the media; the United Nations Independent Expert on Albinism; and other NGOs and CSOs.
MANUAL OF BEST PRACTICE
We have recently compiled and published the Manual of Best Practice: Skin Cancer Prevention and Management for Persons with Albinism in Africa: a ground-breaking resource that will strengthen our provision of training and accelerate replication of the Skin Cancer Prevention Programme in other African countries.
Produced in collaboration with the International Foundation for Dermatology and funded by Novartis and the Fondation Pierre Fabre, this manual is the first ever internationally recognised resource enabling clinicians to deliver effective quality care to patients with albinism, specifically targeting African contexts. It targets consultant dermatologists, surgeons, dermatology officers, clinical officers and nurses and largely draws on the experience of our programme personnel. It aims to consolidate current learning and drive improvements in clinical practice for professionals working to promote the dermatological health of people with albinism in Africa. As a user-friendly tool for change, the manual will help us achieve faster and more reliable replication of the programme internationally. Its French translation will be explicitly mobilised for replication in Francophone countries.
The compilation of the manual was led by the Chairperson of our Skin Cancer Advisory Committee, Dr Andrew Sharp. Contributions were received from other committee members, and global health experts from Tanzania, Malawi, the United Kingdom, the USA and Spain.
Throughout 2018 the manual was field-tested during programmatic interventions in Tanzania and Malawi. In June 2019, it was presented to leading international stakeholders at the World Congress of Dermatology in Milan and a major disability rights conference at the United Nations in New York. Standing Voice’s Skin Cancer Advisory Committee is in the process of developing a training framework based on the manual that will complement this resource. This framework will provide a clear guide and structure for how to train clinicians using our recommended and well-evidenced best practices for preventing and managing skin cancer in people with albinism. This standardised training material will be deployed to accelerate programme replication.

Reach
Our programme currently serves 9,518 patients at 199 locations across Tanzania and Malawi
Impact
From 2017 to 2019, rates of harmful skin conditions fell by 23% across our patient population
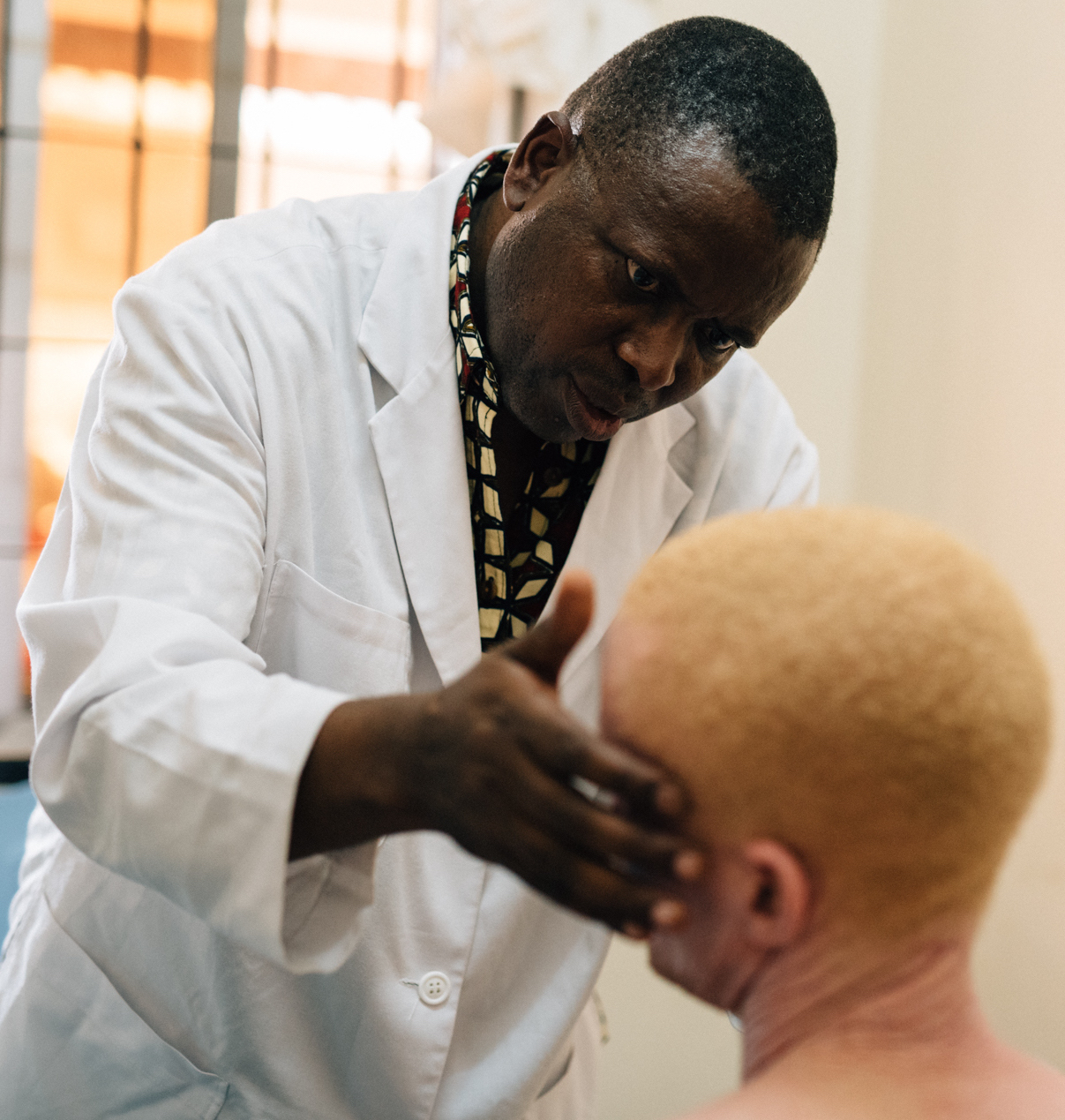



"Standing Voice has given us the power to use our skills as community dermatologists."
Dr Jackson Materu – Dermatologist
"Bringing health services to people with albinism in their own communities is indispensable."
Ikponwosa Ero – UN Independent Expert on Albinism
"It’s incredibly special to see this programme developing transformative clinical practice."
Dr Melissa K Levin – Standing Voice Skin Cancer Advisory Committee Member
"My skin has improved greatly because of Standing Voice."
Vedastus Wilfred – Programme Beneficiary
STORIES




